Analyzing the top 10 causes of death announced by the Ministry of Health and Welfare in 2021, apart from cancer, which continues to account for the highest percentage, heart disease (20,547) and cerebrovascular disease (11,821) are next in line, all of which are closely related to cholesterol and high blood cholesterol. How should we take cholesterol correctly to reduce the risk of diseases?
The misperception of cholesterol
When we hear about “cholesterol,” we may think it is unhealthy or that the less it is in our body, the better. Cholesterol is the raw material needed to make cell membranes and synthesize hormones and plays an essential role in maintaining physiological functions, unlike what is said to be harmful.
The relationship between cholesterol and hyperlipidemia
In general, the indicators of “total cholesterol,” “low-density cholesterol (LDL-C),” “high-density cholesterol (HDL-C),” and “triglycerides” seen in the health checkup report, if the “total cholesterol,” “triglycerides,” and “LDL-C” in the blood are too high, and “HDL-C” is too low. Or a combination of all of the above is called “hyperlipidemia.”
Why are they called “good cholesterol” and “bad cholesterol”?
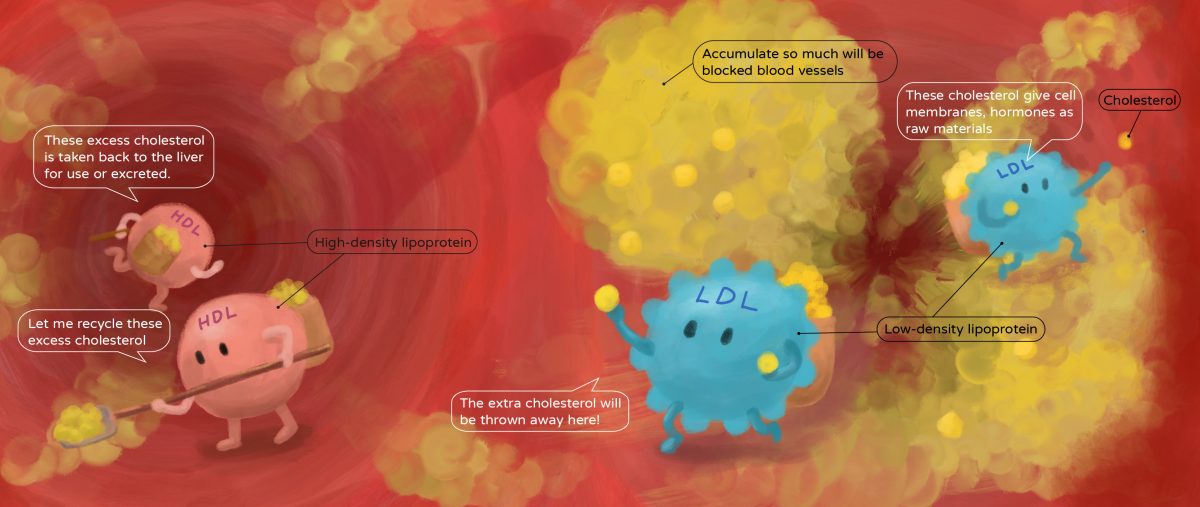
Whether in food or the body, cholesterol is not good or bad “by itself” but rather in how the body uses it. Cholesterol is transported and recycled in the blood vessels by lipoproteins, which distribute cholesterol to various tissues and recycle excess cholesterol to the liver.
We can assume that cholesterol is initially a simple, good person with two good friends: high-density lipoprotein (HDL) and low-density lipoprotein (LDL).
We can consider HDL as the “good friend” of cholesterol and LDL as the “bad friend”; why do we say so?
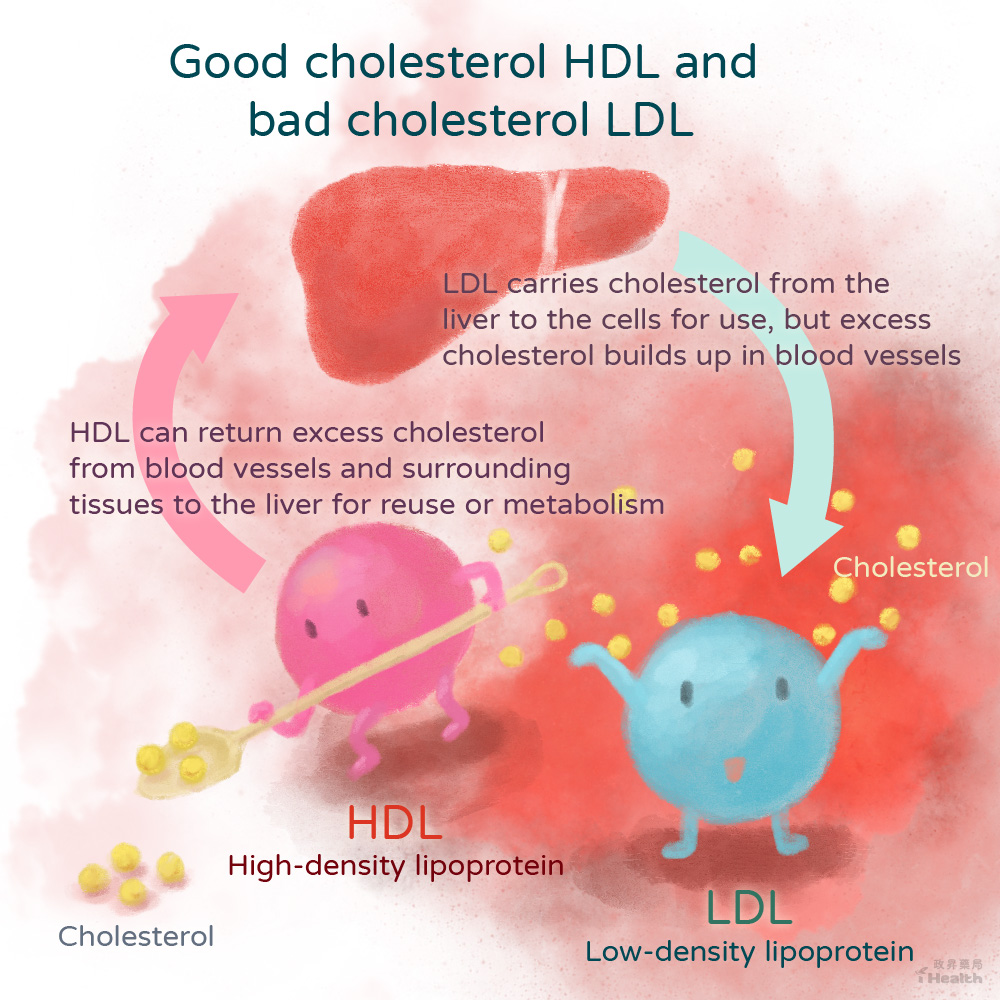
HDL-good cholesterol
HDL can transport cholesterol from blood vessels and surrounding tissues to the liver for synthesis and metabolism, removing excess cholesterol from blood vessels and avoiding accumulation in the vessel walls, which positively affects blood vessel health.
LDL-bad cholesterol
Because of its small size, LDL easily penetrates the walls of blood vessels to form atherosclerosis, causing them to thicken and lose elasticity. The narrowing of blood vessel channels will lead to difficulty in blood flow and, in severe cases, even blockage of blood vessels.
Therefore, the “high-density lipoprotein cholesterol (HDL-C)” commonly seen in health checkup reports is also called good cholesterol. In contrast, “low-density lipoprotein cholesterol (LDL-C)” may cause cardiovascular disease when in excess, also known as bad cholesterol.
Why does it cause hyperlipidemia?
The causes can be divided into two major parts: genetic and acquired factors. Excluding the uncontrollable congenital factors, the following behaviors may trigger hyperlipidemia.
- Disease effects: diabetes, kidney disease, hypothyroidism, liver disease, etc.
- Medications: thiazide diuretics, hypotensive drugs, steroids, oral hormones, etc.
- Bad lifestyle habits: excessive total calorie or fat intake, excessive alcohol consumption, smoking, obesity, low physical activity, etc.
Especially the diet, like eating until full, fried, fatty meat, animal offal, dairy products, delicate desserts, and shelled seafood, are considered dangerous groups of high blood lipids! In addition, long-term life tension, and excessive work pressure, may also lead to abnormal blood lipids.
Where does cholesterol in the blood come from?
When we eat high-cholesterol food such as egg yolk, will it be wholly converted into blood cholesterol, increasing the burden on blood vessels?
Food cholesterol ≠ blood cholesterol
In 2015, the U.S. Department of Agriculture (USAD) published a dietary guideline that eliminated the upper limit of cholesterol intake because studies by the American Heart Association (AHA) and the American College of Cardiology (ACC) showed that the correlation between “cholesterol consumed and cholesterol in the blood” is no longer so absolute.
There are two primary sources of cholesterol in the human body, the liver produces about 70-80%, and the other 20% is taken from food, indicating that the body makes most cholesterol.
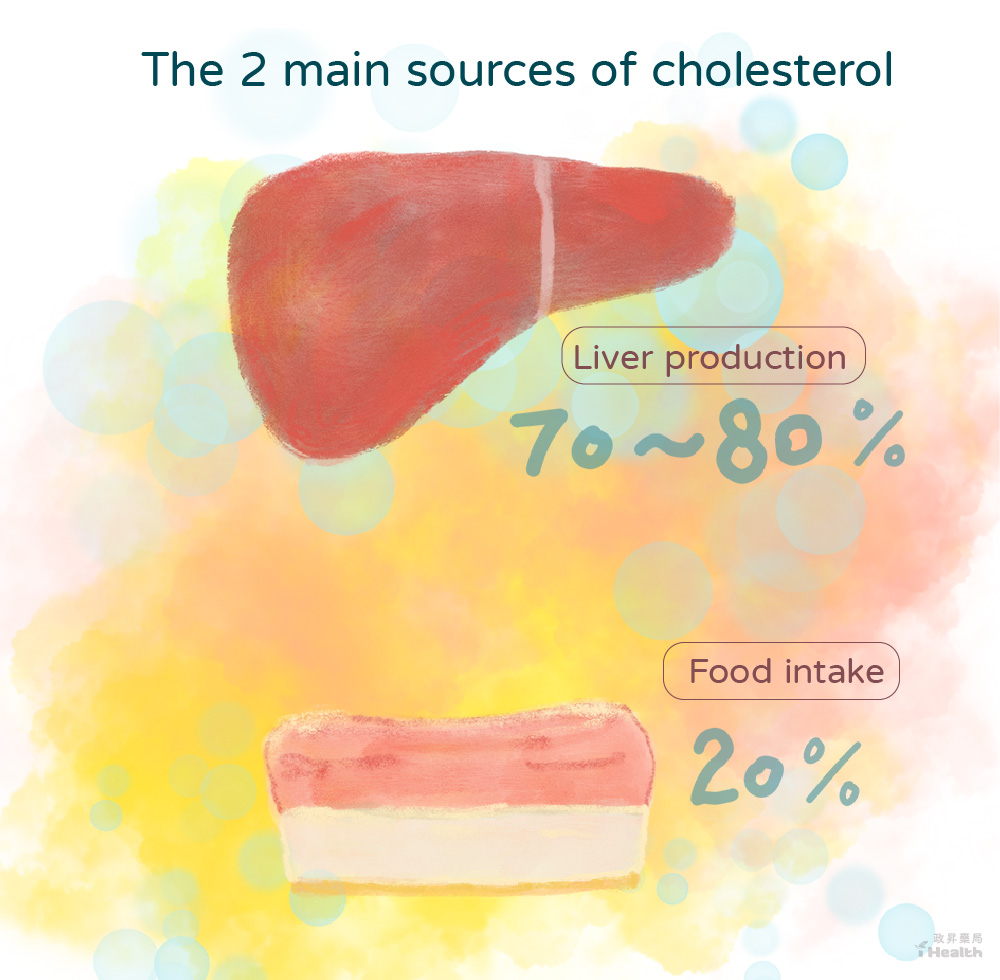
And the body has a set of regulatory mechanisms; once cholesterol intake is too much, the liver will reduce the amount of synthesis so that the cholesterol concentration maintains an average value.
Can we safely eat high-cholesterol foods?
Although cholesterol is not good or bad “by itself,” we should pay attention to other ingredients in food because high-cholesterol foods often contain “high saturated fatty acids” or “high calories,” and saturated fatty acids increase the concentration of LDL cholesterol, which in turn increases the risk of cardiovascular disease.
Therefore, patients with hyperlipidemia, it is not cannot consume high-cholesterol foods, but they should pay attention to the possible adverse effects of other ingredients.
The three keys to lowering and controlling blood lipids
For patients with hyperlipidemia, the following principles help control blood lipids.
Daily habit
- Get rid of bad habits: such as quitting smoking, drinking, avoiding late nights, and maintaining a regular work schedule.
- Increase the frequency of exercise: Exercise helps burn calories and avoid obesity and increases the concentration of good cholesterol in the blood.
- Maintain ideal body weight: BMI control at 18.5~24.
- Maintain emotional stability: Arrange leisure activities appropriately to release stress.
- Regular health checkups: Pay attention to cholesterol and triglyceride values.
- Take medication on time: For patients with hyperlipidemia, medication control is significant, so you should follow the instructions of your doctor and pharmacist to take medicines on time and not stop taking them rashly.
Diet
✕ Avoid
- Foods high in cholesterol: such as animal skin or offal (pork skin, heart, liver, etc.), pork/butter, pork or fatty meat, crab yolk, fish eggs, egg yolk
- Refined sugar: Sweets, sugary drinks, or large amounts of starch can raise bad cholesterol.
- High-calorie foods: High-calorie foods such as fried foods and refined desserts will increase cholesterol absorption in the intestines, which can also easily lead to being overweight.
✓ You can eat more
- Deep-sea fish rich in omega-3 fatty acids: such as mackerel, salmon, okra, tuna, etc., can boost good cholesterol and promote blood vessel health.
- Foods rich in water-soluble dietary fiber: such as bowls of beans, okra, potatoes, oats, barley, bananas, apples, etc. Soluble fiber helps to reduce short-stack cholesterol and bad cholesterol (LDL-C) and reduces the body’s inflammatory response.
✓ Cooking method
- Use more steamed, boiled, chilled, roasted, grilled, stewed, braised, and avoid deep-frying and frying. Choose oils with a high unsaturated fatty acid content, such as olive oil, peanut oil, canola oil, sunflower oil, etc. Stir-fry with water as much as possible and avoid high heat to avoid oil deterioration beyond the smoking point.

Medication
People with dyslipidemia who cannot lower their LDL-C through lifestyle changes may be at increased risk for cardiovascular disease over the long term, so they should receive statins-like medications as soon as possible to provide cardiovascular protection.
A small number of patients may experience myopathy, such as muscle pain, weakness, cramps, stiffness, etc. However, there are still side effects that must be noted with statins. If patients experience muscle discomfort after taking the medication, they should report it to their physician or pharmacist for a medication evaluation.
Although there are no apparent symptoms at the beginning of hyperlipidemia, vascular health is already at risk, so regular health checks are essential! For patients who are already hyperlipidemic, it is crucial to follow the instructions of your doctor and pharmacist to take medication steadily.
Knowing Triglycerides
Triglycerides, like cholesterol, are a type of lipid in the body and come from much the same source as cholesterol. It can provide cells with the energy they need and help store energy. An appropriate amount of fatty tissue can prevent the loss of body heat and protect internal organs to reduce impact and friction.
Suppose the body’s triglyceride concentration is too high. In that case, it will affect the body’s metabolism, leading to high blood pressure, high blood sugar, or high blood fat, and may increase the risk of arteriosclerosis. In addition, triglycerides also tend to make the blood too viscous; if the index ≧ 500 mg / dL, it may cause acute pancreatitis.
Interpretation of Health Screening Reports – Diagnostic Criteria for Hyperlipidemia
| Normal value | Alert value | Hazard Value | |
| Total Cholesterol (TC) | < 200 mg/dL | 200~239 mg/dL | > 240 mg/dL |
| Low-density lipoprotein cholesterol (LDL-C) | < 130 mg/dL | 130~159 mg/dL | > 160 mg/dL |
| High-density lipoprotein cholesterol (HDL-C) | > 40 mg/dL | < 40 mg/dL | < 40 mg/dL |
| Triglycerides (TG) | < 150 mg/dL | 150~199 mg/dL | > 200 mg/dL |
Generally, the cholesterol index should be maintained within normal values. If the test result is at the alert value, the diet and lifestyle should be adjusted and followed up again within a year. If one of these values reaches a risk level and cannot be controlled with diet and exercise changes, it must be controlled with medication.
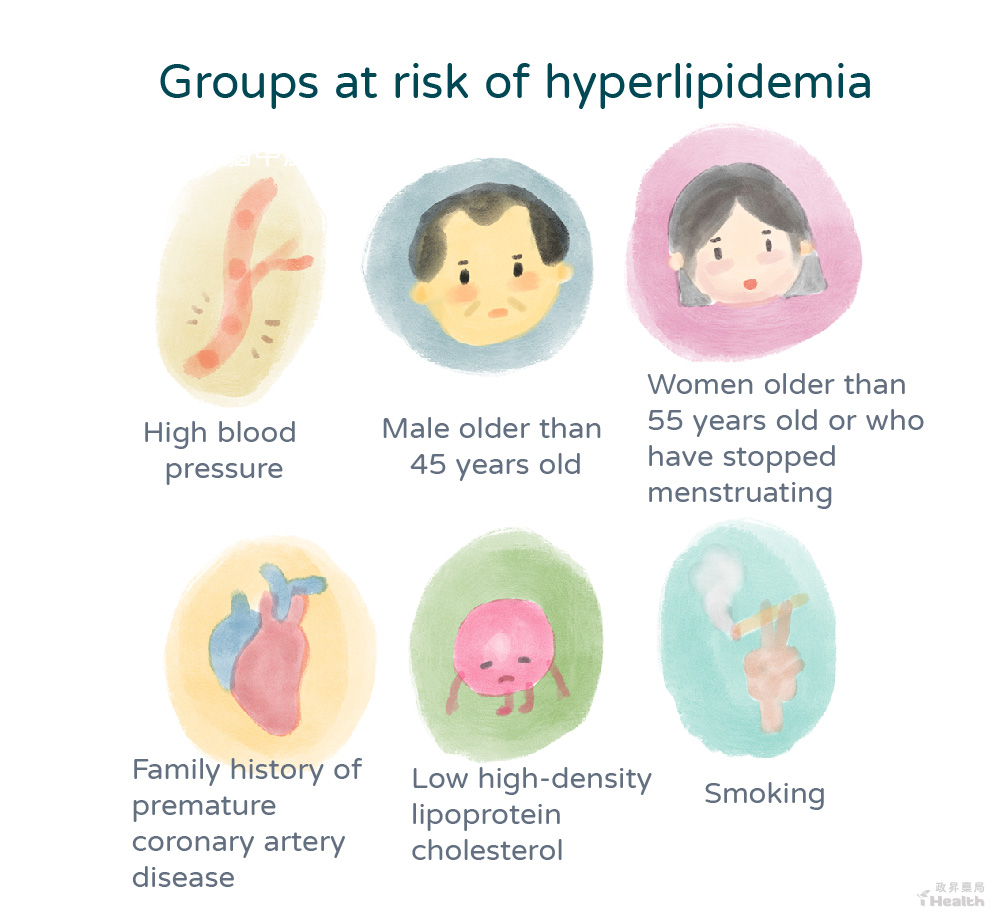
The diagnosis of hyperlipidemia cannot be determined from a single indicator but requires observation of the ratio of various lipid components and a comprehensive assessment by a physician. The presence of risk factors for cardiovascular disease may increase the potential risk to the body, such as
- High blood pressure
- Men older than 45 years old, women older than 55 years old, or menopause
- Family history of premature coronary artery disease (male ≦ 55 years old, female ≦ 65 years old)
- Low HDL cholesterol (HDL-C < 40 mg/dL)
- Smoking
What are the risks of high blood cholesterol?
The most direct effect of high blood lipid concentration is to cause arteriosclerosis or blockage of blood vessels.
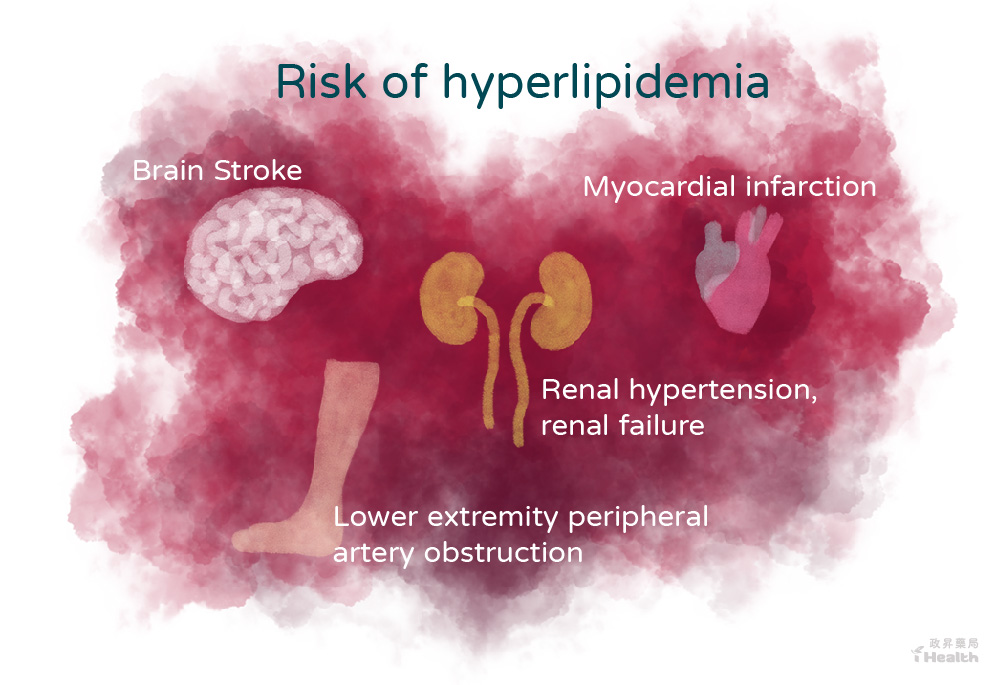
If the blockage occurs in the brain, it may cause a stroke, resulting in permanent damage; if it occurs in the kidney vessels, it may cause renal hypertension and kidney failure; if the blockage is in the peripheral arteries of the lower extremities, it may lead to a decrease in blood flow to the terminal extremities and intermittent claudication (sudden pain, numbness) or other pathologies in the lower extremities.
Suppose the blockage occurs in the coronary arteries near the heart. In that case, it may cause myocardial hypoxia, chest tightness, and angina symptoms. If the sclerotic plaque ruptures and completely blocks the blood vessel, it may cause myocardial infarction. Especially when the temperature changes drastically, myocardial infarction often comes suddenly, and the mortality rate is relatively high.
Therefore, if the blood lipid concentration is not controlled correctly, the health hazards are not to be underestimated.
Reference:
台北榮總、馬偕醫院、三軍總醫院、家庭醫學與基層醫療、膽固醇迷思與反迷思




