

As of June 2022, the number of new coronary pneumonia cases worldwide has reached 535 million, and the number of confirmed cases in Taiwan has officially surpassed 3 million people. In addition, global case reports show that over 80 million people have recovered from the diagnosis but continue to have symptoms of Long COVID.
What is a Long COVID?
According to the current definition of the World Health Organization (WHO), COVID-19 infection within four weeks is called the acute phase, and symptoms that persist or are delayed for 4-12 weeks are known as “Post-COVID-19 syndrome”, or “Long COVID”.
In the current study, the incidence is between 10-20%; although the infection is mild, healthy adults and children can develop Long COVID, and the symptoms are mostly similar.
What are the common symptoms?
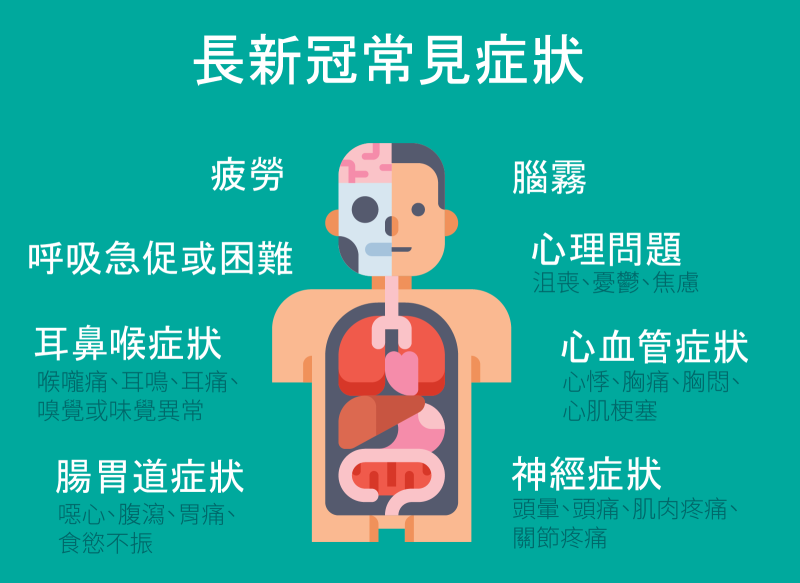
More than 200 types of sequelae are recorded in the literature, such as fatigue, shortness of breath or difficulty, and cognitive dysfunction (e.g., brain fog: inability to concentrate, inability to focus on thinking, poor memory, insomnia, etc.) being the most common.
Other common symptoms include:
- Cardiovascular symptoms: palpitations, chest pain, chest stuffiness, myocardial infarction.
- Gastrointestinal symptoms: nausea, diarrhea, stomachache, depraved appetite.
- Ear, nose, and throat symptoms: sore throat, abnormal smell or taste, tinnitus, earache.
- Neurological symptoms: dizziness, headache, muscle aches, arthralgia.
- Psychological problems: depression, melancholy, anxiety.
The high-risk groups of Long COVID
According to the CDC report, researchers are working to understand who is vulnerable to persistent effects after being infected with COVID-19 and provide the following examples based on current research.:
- People who did not get a COVID-19 vaccine
- People who had underlying health conditions before COVID-19.
- People who have experienced more severe COVID-19 illness, especially those hospitalized or needing intensive care.
- People who experience multisystem inflammatory syndrome (MIS) during or after COVID-19 infection.
Other studies have shown that people with multiple symptoms during diagnosis, older people, smokers, and people with metabolic problems (such as obesity) may have a higher risk of Long COVID.
When should people start worrying that they may have Long COVID?
In March 2022, Dr. Janet Diaz of the World Health Organization’s Clinical and Infectious Diseases Group stated that most patients recover from the acute phase within three months of diagnosis and must be evaluated by a physician if one of the suspected symptoms of Long COVID remains after three months.
What is the duration of Long COVID symptoms?
According to WHO Dr. Janet, if symptoms disappear within a few weeks or a month, it may not be considered Long COVID; if symptoms persist for at least two months, the likelihood of Long COVID is high. In the cases reported so far, the symptoms may last six months or even a year or more.
What are the treatment options?
The condition is different types of symptoms that affect multiple systems of the body, so the treatment is not one treatment for all patients. Instead, the treatment must be patient-centered and focused on the patient’s symptoms.
For example, if the patient is tired, they should reduce activities when fatigued and choose to do them when relatively less tired; if the patient has cognitive impairment, try not to multitask at the same time and try to focus only on the one activity being handled; if the patient has insomnia, the solution is to seek health education from a physician to prevent it.
Although the vast majority of Long COVID is not life-threatening, its symptoms still significantly impact people’s quality of life. Physicians from the WHO recommend that prevention and treatment of Long COVID can be done through a comprehensive assessment of past medical history by community physicians who know us best.
Are the sequelae similar for different virus strains (e.g., Alpha, Delta, Omicron)?
In the case of Alpha and Delta may damage the lung, cardiovascular, and brain nerves. It is worth noting that the virus destroys cells and triggers a “Cytokine Storm,” which puts the body in a highly inflammatory state and damages normal tissues. Studies have confirmed that this strain of the virus has significantly increased the incidence of cerebrovascular disease, arrhythmia, myocarditis, heart disease, and blood clots in patients 12 months after contracting the disease and that neurological damage, neuronal degeneration, and apoptosis have been observed in the brains of post-epidemic monkeys.
In contrast, Omicron, because it mainly attacks the upper respiratory tract and is less likely to enter the lungs, is less likely to cause systemic infection, less likely to cause tissue damage, and less likely to cause Cytokine Storm, so experts estimate that the incidence of systemic sequelae should be theoretically low. However, patients should not ignore the fact that a study in March 2022 found that even in mild cases, brain function may be impaired.
| Alpha | Delta | Omicron | |
| Time/Place of appearance | 2020/09/UK | 2020/10/India | 2021/11/South Africa |
| During the epidemic | 2020/12 – 2021/06 | 2021/03 – 2021/10 | 2021/11 – present |
| Common clinical symptoms | Fever, cough, sore throat, difficulty breathing | Fever, cough, sore throat, runny nose, difficulty breathing | Fever, cough, sore throat, rare loss of smell and taste, milder symptoms |
Many studies on Long COVID are still underway, including whether new vaccines and new antiviral drugs can help reduce the risk of Long COVID, and I believe there will be more answers shortly.
Reference:
WHO – Update on Long COVID
CDC USA – Long COVID or Post-COVID Conditions
Nature Medicine – Post-acute COVID-19 syndrome
Nature – SARS-CoV-2 is associated with changes in brain structure in UK Biobank
Mayo Clinic – COVID-19 : Long-term effects Print
衛福部 – 新型冠狀病毒(SARS-CoV-2)感染臨床處置指引$
衛福部 – COVID-19染疫康復者門住診整合醫療計畫
泛科知識



